Injured Senior Hit by Car Receives Justice and Rare Insurance Reversal
By Peter Defilippis, Esq.
Our client, an 82-year-old pedestrian, faced a harrowing incident when she was struck by a car as the driver carelessly backed up in front of the exit to a gas station convenience store. Emerging from the store’s doorway, she suffered comminuted fractures in three critical areas – her ankle, heel, and mid-foot.
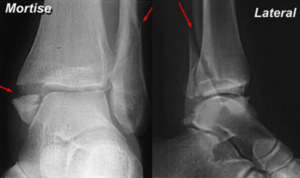 Comminuted fractures, involving bone breaking into more than two fragments, led our client to require extensive medical treatment. GEICO, the insurance company for the car’s owner and driver, was expected to provide coverage. Despite severe impairment in her lower leg and heel, limiting her ability to walk, the insurance company’s doctor conducted a brief examination, concluding no further treatment was necessary. Consequently, her no-fault benefits were abruptly terminated.
Comminuted fractures, involving bone breaking into more than two fragments, led our client to require extensive medical treatment. GEICO, the insurance company for the car’s owner and driver, was expected to provide coverage. Despite severe impairment in her lower leg and heel, limiting her ability to walk, the insurance company’s doctor conducted a brief examination, concluding no further treatment was necessary. Consequently, her no-fault benefits were abruptly terminated.
The orthopedic surgeon who treated our client recommended a triple arthrodesis procedure, but he understandably would not perform the surgery without the presence of insurance coverage. Medicare claimed it was not obligated to cover the cost of the surgery, and likely would have placed an enormous lien on any arbitration recovery if it had paid for it. We wrote several letters to GEICO and the New York State Department of Finance, which has some jurisdiction over New York insurance entities. In the letters, we outlined the situation, provided all our client’s medical details, and pleaded with the decision-makers to reinstate her benefits.
To its credit, GEICO reversed its earlier unfair decision and fully reinstated her no-fault benefits, eliminating the possibility of a lien on any recovery in her case! This was a welcome surprise, but even if GEICO had not done the right thing by reversing its prior decision, we were prepared to pursue other recourse against the insurance company.
Our client bravely underwent triple arthrodesis surgery, but the journey has been challenging. Throughout arbitration, her difficulty walking and discomfort in the witness chair were evident as she relied on a cane. Notably, the arbitrator emphasized her credibility in the written decision. In legal proceedings, arbitrators, judges, and jurors keenly observe a plaintiff’s physical demeanor both in and around the courthouse. The honest and straightforward testimony of the plaintiff remains paramount, influencing the perceptions of jurors and judges in the court of law.
We just received the arbitrator’s decision, awarding our client $250,000 – the full amount of underinsurance coverage! He found she was not negligent to any degree. He went out of his way to write, “Claimant’s counsel did an outstanding job in preparing and presenting the case” and “She would have been entitled to $500,000, in my view, had there been that much coverage.” He even ordered her underinsurance carrier to reimburse her for the American Arbitration Association filing fee.
Our client is undergoing a challenging recovery from surgery, and we earnestly wish her a full and speedy recovery, hoping for relief from her enduring pain. Our firm believes we’ve made a positive impact, ensuring justice in her case.
While we appreciate GEICO’s ability to compromise in this instance, we recognize that such understanding isn’t always the norm with insurance companies. If you or a loved one has suffered an injury in an accident, reach out to us. Our firm, with decades of experience, is dedicated to ensuring fair treatment and optimal resolutions for each client.
The Law Offices of Peter DeFilippis & Associates have been assisting victims of malpractice, negligence, and wrongful death in New York City and Westchester County since Mr. DeFilippis was admitted to the New York State Bar in 1989. We stand ready to help you too. If you’ve experienced a serious injury in an accident, contact us online at [email protected] or call (212) 227-4001 or (914) 478-7777.